Yoga for Immune and Respiratory Health
Feb 12, 2021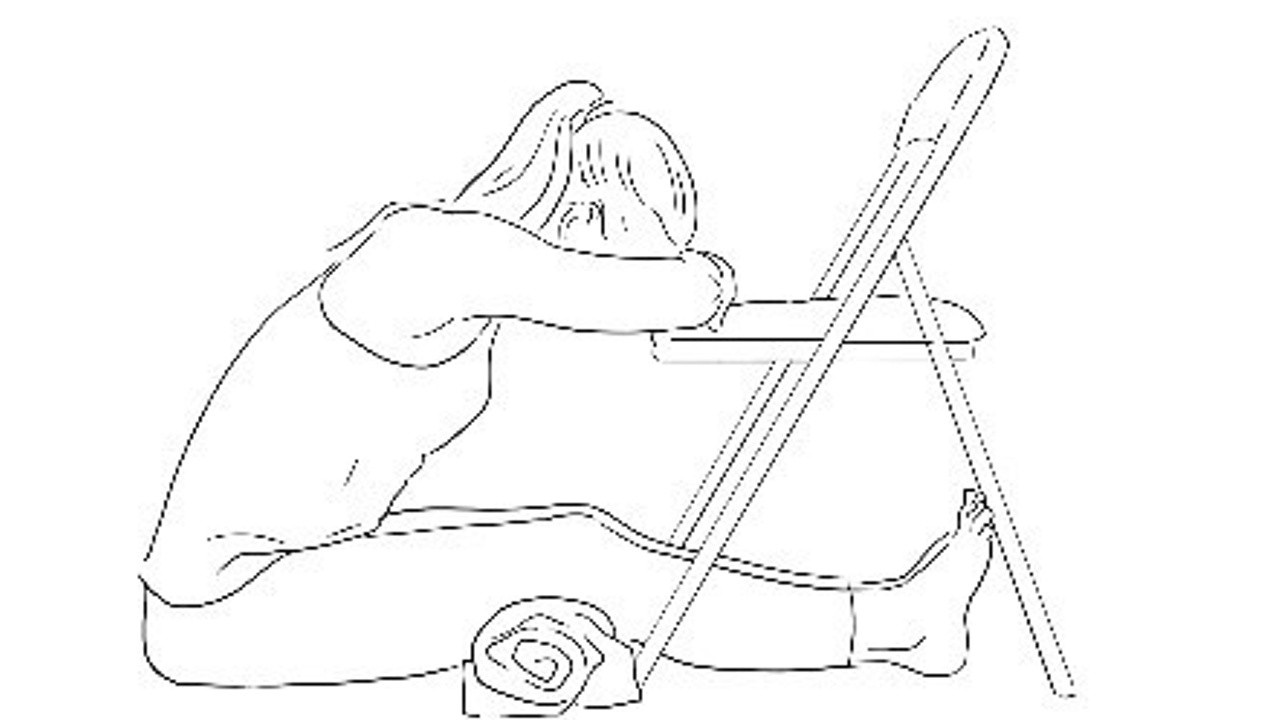
Right now, as we navigate the Covid-19 pandemic, the usual boundaries between the outside world and our internal landscape have shifted in ways we could not have anticipated. Plunged into rapid-response mode, we are fire-fighting; bodies and minds racing to keep up with the most appropriate and effective responses to current threat and danger.
Two body systems at the heart of these responses are the immune and respiratory systems – how we protect ourselves and how we breathe. Given the nature of the coronavirus, these two functions are of optimal interest at the moment – supporting their function may not prevent us picking up or contracting the disease, but how we move, breathe, reduce stress and eat can have an affect on how our immune system deals with it and the severity of symptoms.
While we know that those with pre-existing conditions – immune-based issues (such as respiratory, inflammatory or autoimmune conditions), heart conditions and metabolic issues such as diabetes – may be most at risk, our immune system is intimately and inseparably linked to nervous, digestive, fascial, lymphatic, hormonal, integumentary (skin) and other body systems. From a holistic (or systemic) viewpoint, rather than a reductionist one, we should consider our entire body (and mind) as a symbiotic network that can either be operating in harmony or with discord.
Understanding how this effects our immune system – the basis of our defence and protection, but also healing and rebuilding – is key to our ability to move through difficult times, both physically and emotionally.
Breath and the nervous system
Our breath is part of the autonomic nervous system – the bit that gets on with basic body functions without us needing to get consciously involved. This means that it changes in response to the rest of the nervous system and in particular, to signals of real or perceived danger. When we go into the more self-protective ‘fight-or-flight’ mode (aka stress), its rhythm speeds up to meet the increased energy release, heartrate, mental acuity and oxygen to muscles that are deemed necessary for us to survive in a potentially hostile situation.
Immunity and the nervous system
In terms of the immune system, short term stress causes an immune system boost, both to activate inflammation to stop us bleeding to death if wounded and to bring immune components to any injury to prevent infection; highly life-threatening in the wild where there are no antibiotics.
As a stressful situation continues, physical processes happen to help us adapt. Take extended pressure at work; under increased mental demands, the body will instinctively release more stress hormones to help us stay focused. Meanwhile the immune system is suppressed, sparing energy for the tasks at hand. If this is in response to feeling unsafe or unsettled at work, home or generally in the world, the response is physiologically similar, but may come with anxiety that ramps up into hypervigilance. Either way, breathing can become shallower at an attempt to feed the brain with more oxygen to keep us going. For humans, our brains are the main organ of survival and they use up an astonishing 70-80% of energy expenditure when we are stressed; compare this to just 20% at resting, calm states and you can see how stress wears out resources and puts a strain on all systems.
When stressful situations continue for more than a few weeks (chronic stress), your body, which began by resisting the stress with gusto, begins to lose its adaptive capacity. This will manifest differently in different people, which is where we can see different ‘stress-related’ symptoms in individuals.
Immune and respiratory conditions
For many, the immune system may get stuck in inflammatory mode, leading to stress-related skin, joint and/or digestive problems while the body’s ability to fight invading bacteria or viruses is chronically suppressed. Continual sore throats, sniffles or cold sores are warning signs. People with long-term stress may succumb to severe infections, autoimmune conditions, increased blood pressure and heart attacks due to this poor immune modulation. Atopic conditions are those where familial traits tend to these inflammatory conditions such as eczema, dermatitis, hayfever, migraines and asthma.
These patterns can also get stuck as immune issues within the respiratory tract, with tendencies to upper respiratory tract infections, susceptibility to bacterial infection such as pneumonia and of course, more severe symptoms in a virus such as Covid-19. Stress also interferes with circulation, keeping blood pressure high to maintain fast oxygen delivery to tissues expecting to move rapidly in self-survival reactions. This can be a causative factor in pulmonary (lung) conditions such as pulmonary embolism (blockage in an artery in the lungs) and pulmonary hypertension (narrowing of arteries in the lungs).
Mindful movement: key to less stress, smoother breathing and greater immunity
At a time of environmental (societal) as much as personal stress – both real and perceived – creating a regular routine that includes self-care is vital to support our immune and respiratory systems; via nervous system regulation. But these are not isolated from other body systems; all are interconnected – like a symphony – and are in constant interplay with every other. For instance, the lymphatic, digestive, detoxification, integumentary (skin) and endocrine (hormonal) systems are all responding to external stimuli and internal voices (eg worry and fear) to mount whole body change and response.
We are designed for this constant orchestration of highs and lows, but system get overloaded when chronic stress or trauma keeps us in heightened states of ‘constant alert’ and we get little chance to let all of the spinning plates come down into rest, recover and renewal modes. This is chicken-and-egg stuff; all of these immune responses affect the respiratory system. From there, the affected nature of the breath feeds into the nervous system and back to immunity.
This is where yoga practices come in to allow us to self-soothe and bring consciousness, calm and ease to these states of survival. As this readiness is mobilising and agitating, it can involve busy and racing mind states, as well as tendencies to judgment and attachment to solving and fixing. Making space for an embodied movement practise creates a safe retreat in which we can ‘drop down’ from the state of alarm and all systems prepped to respond to danger. Mentally we can drop away from going round and round in fear-based mental states and rather drop into embodied awareness – noticing how we are feeling throughout our whole being, in the present moment.
While we do not seek to suppress or ignore the gravity of the unfolding situation, we are encouraged to recognise that in the present moment, for the duration of your practise, you are safe. In yoga we have a particular focus on the breath, the place we have the chance to affect the nervous system and bring down heightened responses, and allow healing.
Mindful movements allow us to tune into and recognise habitual stress response as it happens, and rather than react, respond more calmly. We might notice more and more as we become familiar with breathing or movement practices. For instance, that when we are stressed our breath becomes tight and locked upwards into the chest and shoulders, rather the breathing patterns of more relaxed states, where the diaphragm and belly move more fluidly. The movements we explore here encourage heightened nervous and immune responses to release by facilitating lower and mid torso mobility, and the breath. Shoulder, neck and lower back pain, tight jaws and headaches are just some of the physical symptoms of stress that can be reduced through these movements.
Movement into the protective lymphatic system
For our bodies to effectively release toxins, our lymphatic system needs to work smoothly. Bacteria and protein are removed from the body through the silvery web of lymphatic vessels that runs just under the skin. Lymphatic fluid (lymph) delivers these foreign and toxic agents to nodes in our neck, throat, armpits and groin to be killed and destroyed. The lymphatic ducts drain into the upper chest, the outside of the collarbones and back to the blood pumping via the pulmonary circuit. Overburdened lymph nodes can prevent us dealing with other diseases that enter our bodies, leaving us more open to attack.
Unlike blood, which is always being pumped by the heart to the peripheral body, lymph moves inward and can only move when we do. When we don’t move enough, lymphatic fluids stagnate, which can compromise our immunity. The functionality of our immune system is dependent on our maintaining fluid, pliable soft tissue in the body. Inflammation and fascial adhesions occur when we become tense, immobile or traumatised and normal motility through joints and organs is interrupted.
Good lymphatic drainage is facilitated by movement at the diaphragm, hips, shoulders and neck, effecting our resilience to attack. Furthermore, important lymphatic sites (Peyer’s patches) lie in the gut lining, between its cells. The immune responses in our gastrointestinal tract, signalled through beneficial gut bacteria (probiotics) in the gut microbiome are further compromised by stress. So mindful movement can have a profound effect on our gut health, too.
Breathing that includes diaphragmatic movement is crucial for the lymphatics to move around this mid-body area and from there, up towards the collarbones, neck and throat, and down towards the colon and groin. The shallow or upper-chest bound breath of chronic stress neither allows this, nor fully inflates the lungs and moves intercostal muscles between the ribs for full, oxygenating breath. The commonly collapsed chest of modern postural slumping and looking down at smartphones simply adds into this lack of movement at the chest and diaphragm; also the heart centred area of self-care and compassion.
The importance of slowing down movement
While aerobic activity can be hugely beneficial for overall health, the balance of our body systems (homeostasis) is dependent on movement that helps us tune into our nervous system, to self-regulate. At times of stress, when our systems are already overloaded, harder and faster may deplete rather than replenish. Where our usual gym, cycling, running routines may habitually reduce stress, at these heightened times, quieter, more internally focussed practises may be more appropriate for releasing tension, reducing inflammatory responses, allowing detoxification, and supporting appropriate immune modulation and expression.
Although we may perceive much yoga and t’ai chi as soft and gentle, both foster strength, balance, focus and breath. The inherent mindful focus on breath and body sensation in these practises have been proven to help reduce the anxiety and rumination that can keep us in the stressed states that so deplete or skew our immune responses; with one review stating, “(showing) improved regulation of the sympathetic nervous system and hypothalamic-pituitary-adrenal system in various populations.” Psychoneuroendocrinology.2017;86:152-168)
A study that reviewed nervous system responses (sympathetic and parasympathetic) in relation to markers for immune health (innate and adaptive), but also stress levels (as Heart Rate Variability), blood pressure, and body mass index (BMI), found great improvements over 10 weeks of yoga practice – as well as improvements in physical fitness and strength (Evid Based Complement Alternat Med.2018;2018:6351938).
Another study concluded that ‘yoga can be a viable intervention to reduce inflammation across a multitude of chronic conditions’. Although a review of 15 primary studies covering the Impact of Yoga on Inflammatory Biomarkers (Biol Res Nurs.2019;21(2):198-209 revealed considerable variability in yoga types, components, frequency, session length, intervention duration, and intensity, most reported positive effects on lowering inflammation markers (most commonly interleukin-6, C-reactive protein and tumour necrosis factor), increasing with the amount of yoga practiced.
Adding in touch for oxytocin release
When we offer ourselves (or receive from others) loving touch, a hormone called oxytocin is released from the pituitary gland in the brain. This hormone has been found to reduce levels of fear by reducing the activity of the amygdala, the (lower) mammalian centre of the brain responsible for detecting danger and reacting to perceived emergencies. This activates the soothing branch of the vagus nerve (the ventral vagus) within the autonomic nervous system, that switches off inflammatory processes and allows smoother, deeper breathing.
Oxytocin is also known as the ‘bonding hormone’ as it opens our capacity to connect and feel bonded with others, reducing stress hormones like cortisol and elevating mood. When we are less able to receive a hug from others, offering ourselves loving touch is a direct way of self-soothing, bringing us into our bodies and engaging interoception to shut off left brain chatter. Oxytocin is released after about 20 seconds of sustained touch and we can introduce this into our yoga practice in many ways eg places our hands on our hearts or bellies at regular intervals, or wrapping our arms around our chest (eg lying or sitting) offers us a palpable gesture of loving-kindness.
Immune-Supporting Home Practise
This sequence combines elements of yoga and T’ai chi, bringing attention to smooth, steady breath and full exhalations can help prevent us rushing through on panic mode and help bring us back into a state of kindness and connection to yourself. From a body psychotherapy viewpoint, clearly distinguishing between our internal and external worlds can help boost our resilience to stress, our means of emotional and physical self-defence. Helping to redefine clear boundaries in this way allows us not to feel overwhelmed by situations and the perceived pressures, whether real or imagined – we can come back to our breath and body as a clear refuge in the present moment.
The release of bound up tension in the body starts by coming back to the ground, letting go, releasing from the pull of gravity. We move into standing postures to strengthen and create space, and then ease blood flow to the heart, lymphatic movement through the fascia and viscera and out to the periphery, and back through restorative poses. By positioning our hips above our head to rest at the end, we improve lymphatic flow from the legs back up the body, ensuring the body can completely release what can become stuck in fascia and viscera.
Feel free to explore and add in anything you feel works for you. Also, slow your practice down to include pauses to integrate the effects, bring kind attention to breath and time to register the self-compassion our bodies need to be able to self-regulate.
All-fours – freeing up body tissues
From all-fours, move in any way that feels good through the shoulders, hips, neck and ribs. Also moving into the face, neck, jaw, and eyes and releasing any sighs, yawns, noise or other expressions of nervous system release.
From all fours, then rotate the tailbone in each direction for a few minutes each, feeling how this loosens tissues in the pelvic floor, diaphragm, throat and back off the skull.
All-fours, lifting leg in turn for free exploration
Lifting each leg at a time to explore any free movement, letting the elbows bend as needed to be able to move through all planes available from the places you are rooted; there is no right or wrong here, just feel your body letting you know what it needs.
Downwards-facing dog to ‘puppy pose’
Lengthen out the spine by pushing back and up from open palms to downwards-facing dog. Keep the heels as high as you need to open the front body between the breastbone and the pubic bone. Drop your knees to beneath the hips, to rest your head and elbows to the ground. This position is also a softer alternative to downwards-facing dog.
Curling up and down to standing
Walk your hands back into a squat with the heels up, curled into to a vertical foetal position. From there, bring the heels down and hands off the ground to curl upwards to standing. Come up and down several times before standing feet hip-width apart.
Swinging twist
Between all of the standing movements, loosen tissues around the central body and diaphragm. With soft knees swing the arms around the midline of the body, feeling the movement come from the belly; hands like weights at the ends of arms as ropes.
Standing spine undulations
From standing with knees bent, exhale to curl-in to your front body, whilst reaching the arms forward, inhale to draw the arms back and open the front body. Keep your knees bent to allow movement and even squat down lower on the exhale if comfortable for your knees.
Wide horse stance undulation
Step into a wide-legged stance, feet turned out about 45 degrees from the centre. Inhale to come up, as you open out your arms, exhale to lean your torso forward, taking your arms in the shape of a large ball around the head. Engage your belly as you lengthen your tailbone away from the crown of your head. Move between the two, gathering up through the belly as you inhale back up.
Wide horse stance arm sweep
From the wide stance, begin by sweeping both hands in semi-circles side-to-side as far as shoulder height. Then open out the arm reaching across the body over and out away from the other, holding the space around the ear. Sweep it back and then both arms all the way to the other side and open up there, moving that side-to-side.
From there, come to any standing practice that feels appropriate.
Wide stance twist
Place your fingers onto the ground or a chair and feet parallel, as wide as comfortable for your knees. Explore shifting weight side-to-side and deeply bending one leg, lifting that heel. Begin to lift the same arm as bent leg, reaching with a bent arm for ease through the shoulder as you move side-to-side.
Prasarita Padottasana – full or supported
Opening up channels of the legs for lymphatic action and strong legs giving signals of safety to the nervous system. Head dropping to allow the nervous system to slow, with soft eyes and jaw for smooth, spacious breath and a focus on the soothing exhalation.
Supported, restorative forward bend
Allowing the nervous system to come to rest, the breath to settle and a sense of ‘surrender’ as the front brain and weight of the head is supported.
Ardha Matsyendrasana
A twist with compression into the belly that encourages lymphatic movement around the lower abdomen, groin and inner legs. Also add in a counter-rotation with the neck (looking over the front leg as you continue to turn the chest away) to encourage lymphatic drainage through the collarbone area from nodes in the throat and neck.
Supported full inversion
Support the lower back fully and comfortably with a bolster or stack of towels, with the lower legs able to fully drop onto a chair seat. Close your eyes to move inwards and feel your breath and heart rate naturally slow down. Here the chest is supported open for easeful breath as the heart has to work a lot less and the lymphatics are also more easily able to draw back up to the heart through the reversed effects of gravity.
Supported Savanasana
This is the most important part of the practice, where the movements before are able to integrate into body and mind, allowing us to fully register how we can come to equilibrium; sattva – on the mat and within our lives. It can also be done as a stand-alone practice or after the laying movements at the start of the sequence here; especially if you need support through anxiety or hypervigilance.
Coming to a position where you can fully relax, completely held by the ground. This is where the movements and awareness from the practice can be integrated and assimilated into your immune, nervous and other body systems.
Find further details on Charlotte’s online course with Yogacampus, Teaching Yoga for Immune and Respiratory Health here.




